

Smooth and seamless as a summer breeze
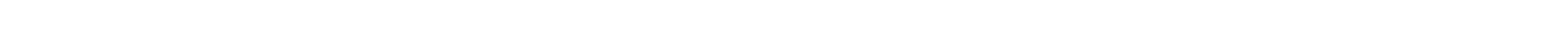
Impact could only be actualized if we improved the claims experience. We've been obsessing over this since day one. After six years of investments, both incremental and impactful, we’re proud to share that Plum’s claims experience is the best in the world.
See it in action.
Your doctor recommends a minor procedure requiring a week's admission, and suggests you get
pre-authorisation approved.
Pre-authorization lets your insurer review the treatment in advance, so you don’t have to pay daily hospital expenses out of pocket, and gives the insurer a heads up on your case, treatment, and length of stay.

Handling paperwork & filing
TIME SAVED WITH PLUM

You hunt for your policy document, health card, and network hospital details, then attempt to complete paperwork with no clarity.
Takes you 3 hrs.

You raise a cashless request on the app, get a call from our support team, and complete basic admission forms. We guide you through the rest.
Takes you 45 mins.
Waiting for approval
TIME SAVED WITH PLUM

The hospital notifies the insurer, but no one follows up. The day ends before pre-auth comes through — you pay for your first day out of pocket.
Pre-auth is approved after seven hours.
Takes you 7 hrs.

As you settle into your room, the Plum team notifies the insurer, coordinates with the hospital, and expedites the process.
Pre-auth is approved within the hour.
Takes you 45 mins.
You spend a week in the hospital. After morning rounds, your doctor okays discharge. You plan to leave after lunch.

Final paperwork
TIME SAVED WITH PLUM

The hospital sends your claim details to the insurer and waits for their response.
Takes you 30 mins.

You notify Plum Care. They work with the hospital to upload all documents and follow up with the insurer.
Takes you 10 mins.
Insurer queries
& clarifications
TIME SAVED WITH PLUM

The insurer seeks clarifications from the hospital. The person at the desk misses the email. An hour later, you check in yourself.
They read it and begin preparing a response.
2 hrs gone.
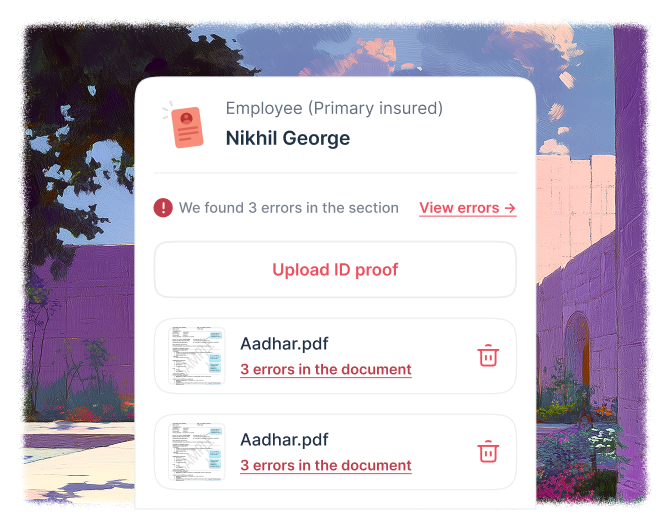
The insurer seeks clarifications. Plum's Claims Router flags the query and initiates a conversation between hospital and insurer.
A team member calls to tell you they're on it.
15 mins, tops.
Handling paperwork & filing
TIME SAVED WITH PLUM

The insurer approves your claim an hour later. You close your account at the desk — four hours since discharge approval.
You get home hoping you didn’t miss dinner.
Takes you 4 hrs 30 mins.

As you receive medication instructions, your claim gets approved. Formalities done in under an hour.
You're home for your post-lunch siesta.
Takes you <50 mins.
You're back home, recovering well. You have bills from post-hospitalisation procedures you'd like to reimburse.

Notifying the insurer and uploading documents
TIME SAVED WITH PLUM

After emailing the insurer and waiting a day for access, you spend hours gathering, scanning, and uploading bills one by one.
Takes you 1 day 6 hrs.

You open the Plum app, raise a reimbursement claim, scan and upload documents using your phone, and click submit.
Takes you <30 mins.
Finding and fixing errors
TIME SAVED WITH PLUM
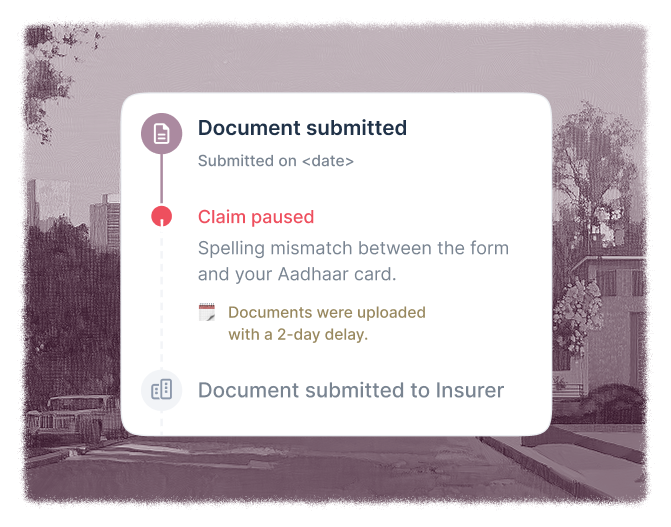
You discover a spelling error a week later. Fix and reupload. Another week before you learn about a missing scan.
Two hospital trips, two weeks lost.
15 days gone.
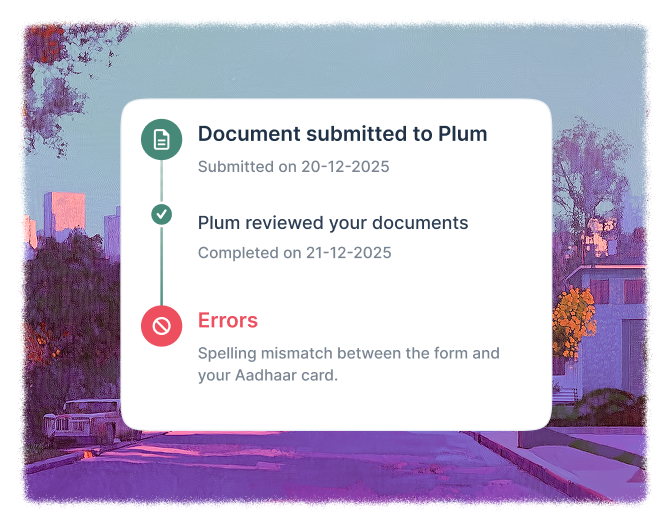
Before you hit submit, you're informed of two errors — a spelling mismatch between the form and your Aadhaar card, and a missing scan.
One hospital visit the next day, and done.
Takes you 1 day 6 hrs.
Contesting a rejected claim
TIME SAVED WITH PLUM

The insurer sends a rejection. After 3 follow-ups and an angry phone call, you learn the reason — and are advised to get a no-objection letter from your doctor.
You plan to go the following week.
Takes you 25 days.

The insurer rejects your claim — treatment was 'not necessary'.
The Plum team is notified, lets you know, and reassures you they're contesting it.
Takes you 1 day 6 hrs.
Bank verification
TIME SAVED WITH PLUM

The claim is approved, but your bank account needs verifying with a cancelled cheque. More delay — you dig out your cheque book and email it over.
Takes you 27 Days.

Your claim is approved within a day. Plum deposits a rupee via Penny Drop to verify your bank account.
Takes you 2 Days.
You receive
your money
TIME SAVED WITH PLUM

Your money arrives almost a month after you started the process.
Takes you 28 Days.

Your money arrives a couple of days after you start the process.
Takes you 2 Days 18 hrs.
best claims experience in
the world
Cashless claims on Plum take half the time to get resolved. Reimbursement claims are closed 10x faster. All with a Claims NPS of 79, the highest in the world.*

It still takes the industry a few hours today.
The industry benchmark is <20%
We ensure fair payouts. ₹10 Cr recovered from denied claims last year.
We’ve made the experience so simple that 1 in 5 people raise claims for out-of-pocket expenses as low as ₹5000.
The fastest end-to-end health insurance claims experience, perhaps on the planet itself.
Only a quarter of the claims we process today require human intervention. Not only does this translate into a seamless experience, but directly impacts the speed of your claim.
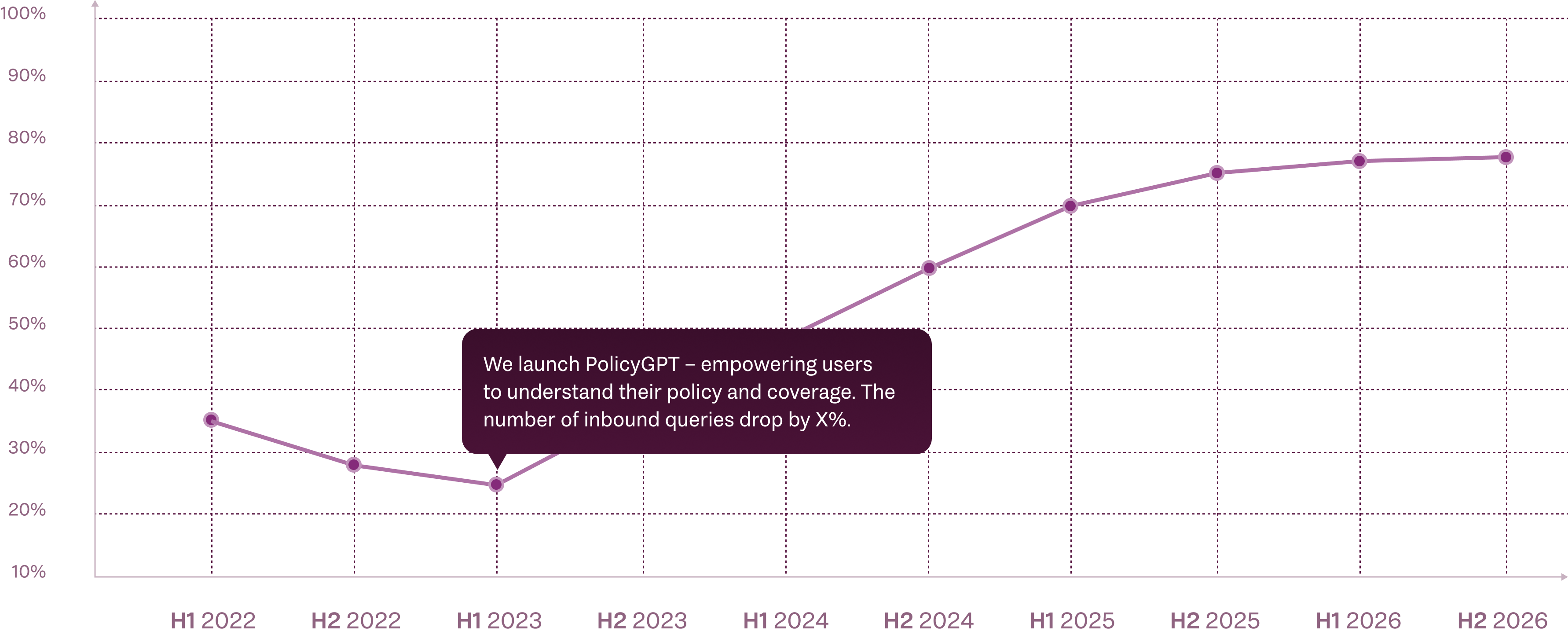
PolicyGPT Launched
Users understand their policy & coverage. Inbound queries drop.
Claims Lens Launched
OCR flags errors before submission. 2x faster resolution.
Claims Router Launched
Proactively flags stuck claims before you know.
PennyDrop Launched
Bank verification without uploading a cheque leaf.
ClaimsLens B&R Launched
Co-authored claims, first-time-right scans.
This is precisely why the biggest team at Plum is not our product or sales teams, but our care team.





.avif)









.avif)





.png)


